The Sneeze Reflex Part II
-From Allergens to Sunshine
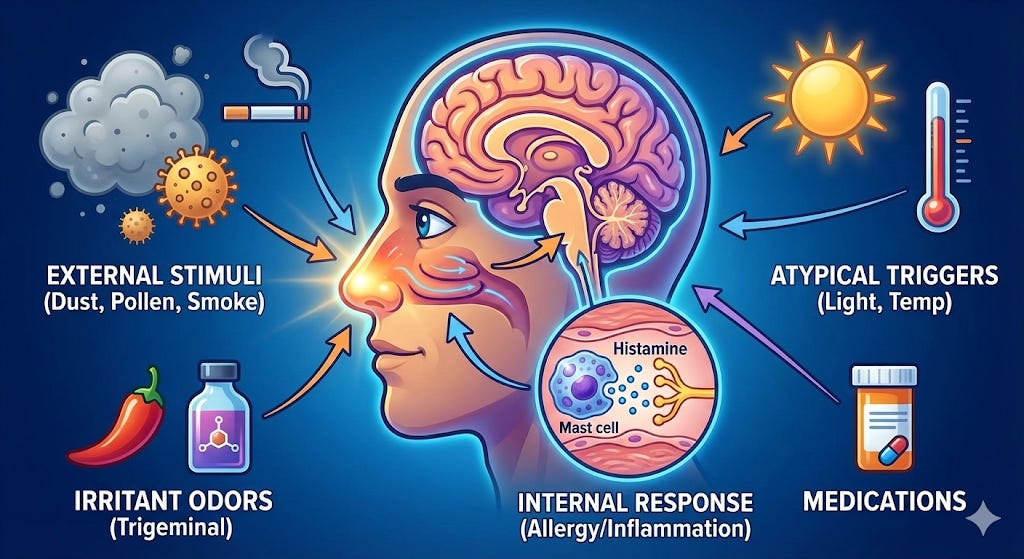
Get ready for the Trigger Gallery! We’ve seen the explosive power of the sneeze, but what actually pulls the pin on the grenade? It turns out, your body has sensors for everything from chemical warfare to a sunny day!
The Usual Suspects: External Stimuli
Your nose is like a high-tech security gate. It uses two different “security teams” to identify intruders:
Team 1: The Trigeminal Nerve (The Pain Police): This team reacts to irritating “heavy hitters” like capsaicin (the heat in chili) and ammonia. When they show up, this nerve sends signals of stinging or burning, which triggers an immediate “get it out!” sneeze.
Team 2: The Olfactory Nerve (The Scent Specialists): These guys handle the non-irritating smells, like PEA (phenylethyl alcohol- the scent of a rose like). While they are usually just there to enjoy the aroma, they can still nudge the sneeze reflex into action if the scent is strong or unfamiliar.
The Hybrid Hits: Most things we smell, like wood smoke (guaiacol), actually set off both teams at once, giving your brain a double-whammy of information!
The Inside Job: Allergies and Infections
Sometimes the trigger isn’t a cloud of dust; it’s a full-blown internal rebellion.
Allergy Alert: When allergens like dust mites or pet dander enter the chat, they damage your “barrier” cells. This activates the mast cells (remember our myeloid heroes?). These cells explode with histamine, a chemical that causes inflammation and forces a sneeze to clear the area.
The Viral Hijack: Viruses and bacteria cause inflammatory reactions that act like a “hair-trigger” on your nasal receptors, making you sneeze at the slightest touch.
(Made Via OpenAI)
The Wild Cards: Light, Temperature, and Meds
Not every sneeze comes from something you inhaled. Sometimes the body’s wiring is just... creative.
The Sun Sneezer (ACHOO Syndrome): For some, walking into bright sunlight is an instant trigger. This is an inherited trait where the visual cortex and the sneeze center seem to share a phone line.
The Thermal Shock: A sudden blast of freezing winter air or steam from a hot shower can shock your nasal receptors into a reflexive “reset” (a sneeze).
The Pharmacy Factor: * The Dampeners: Drugs like antihistamines or fentanyl (used in anesthesia) can quiet the “sneeze alarm.”
The Double-Agents: Some meds, like NSAIDs (painkillers), can actually trigger a sneeze in sensitive individuals as a side effect.
Sneezing may feel simple, but it’s a precisely coordinated defense linking sensory nerves, immune signals, and the brain. Whether triggered by allergens, infections, or even sunlight, this reflex exists to protect your airways from harm. Behind every “achoo” is a rapid, intelligent decision your body makes to keep you safe.
………
On personal note, recently I completed my second 10K RUN or Marathon, but this time I ran after my post ankle injury,. Marathon was good, it took 1 hr 25mins to complete my 10K run, still feel I could’ve done better…but we move onto the next target maybe 21K or more let’s see..I’ll write more about my experience form 10k run in my another substack-
Let me know if you’ve any doubts……….
References-
Badran B. W., Gruber E. M., O’Leary G. H., Austelle C. W., Huffman S. M., Kahn A. T., et al. (2022). Electrical stimulation of the trigeminal nerve improves olfaction in healthy individuals: A randomized, double-blind, sham-controlled trial. Brain Stimul. 15 761–768. 10.1016/j.brs.2022.05.005
Doty R. L., Brugger W. E., Jurs P. C., Orndorff M. A., Snyder P. J., Lowry L. D. (1978). Intranasal trigeminal stimulation from odorous volatiles: Psychometric responses from anosmic and normal humans. Physiol. Behav. 20 175–185. 10.1016/0031-9384(78)90070-7
Eriksen E., Afanou A. K., Madsen A. M., Straumfors A., Graff P. (2023). An assessment of occupational exposure to bioaerosols in automated versus manual waste sorting plants. Environ. Res. 218:115040. 10.1016/j.envres.2022.115040
Gabriel M. F., Postigo I., Tomaz C. T., Martínez J. (2016). Alternaria alternata allergens: Markers of exposure, phylogeny and risk of fungi-induced respiratory allergy. Environ. Int. 89-90 71–80. 10.1016/j.envint.2016.01.003
Calderón M. A., Linneberg A., Kleine-Tebbe J., De Blay F., Hernandez Fernandez de Rojas D., Virchow J. C., et al. (2015). Respiratory allergy caused by house dust mites: What do we really know? J. Allergy Clin. Immunol. 136 38–48. 10.1016/j.jaci.2014.10.012
Hakim K. Y., Alsaeid M. A. (2019). Comparative study between the efficacy of fentanyl, antihistamines, and dexmedetomidine in suppressing photic sneeze reflex during peribulbar block. Anesth Essays Res. 13 40–43. 10.4103/aer.AER_174_18
Tamura T. (2011). Investigation of the antiallergic activity of olopatadine on rhinitis induced by intranasal instillation of antigen in sensitized rats using thermography. Asia Pac. Allergy 1 138–144. 10.5415/apallergy.2011.1.3.138
Yonghua S., Mehrabi Nasab E., Liuo Y. (2022). Effect of temperature and humidity on the allegro-inflammatory factors and allergic rhinitis-related behavior. Iran. J. Allergy Asthma Immunol. 21 704–710. 10.18502/ijaai.v21i6.11531
Parker J. D., Reid P., Bailey M. (2023). The effect of fentanyl coadministration on sneezing during nasal local anesthetic injection for plastic surgery under propofol-based intravenous sedation: A retrospective case-controlled study. J. Opioid. Manag. 19 165–170. 10.5055/jom.2023.0771
Bindu S., Mazumder S., Bandyopadhyay U. (2020). Non-steroidal anti-inflammatory drugs (NSAIDs) and organ damage: A current perspective. Biochem. Pharmacol. 180:114147. 10.1016/j.bcp.2020.114147




So well written